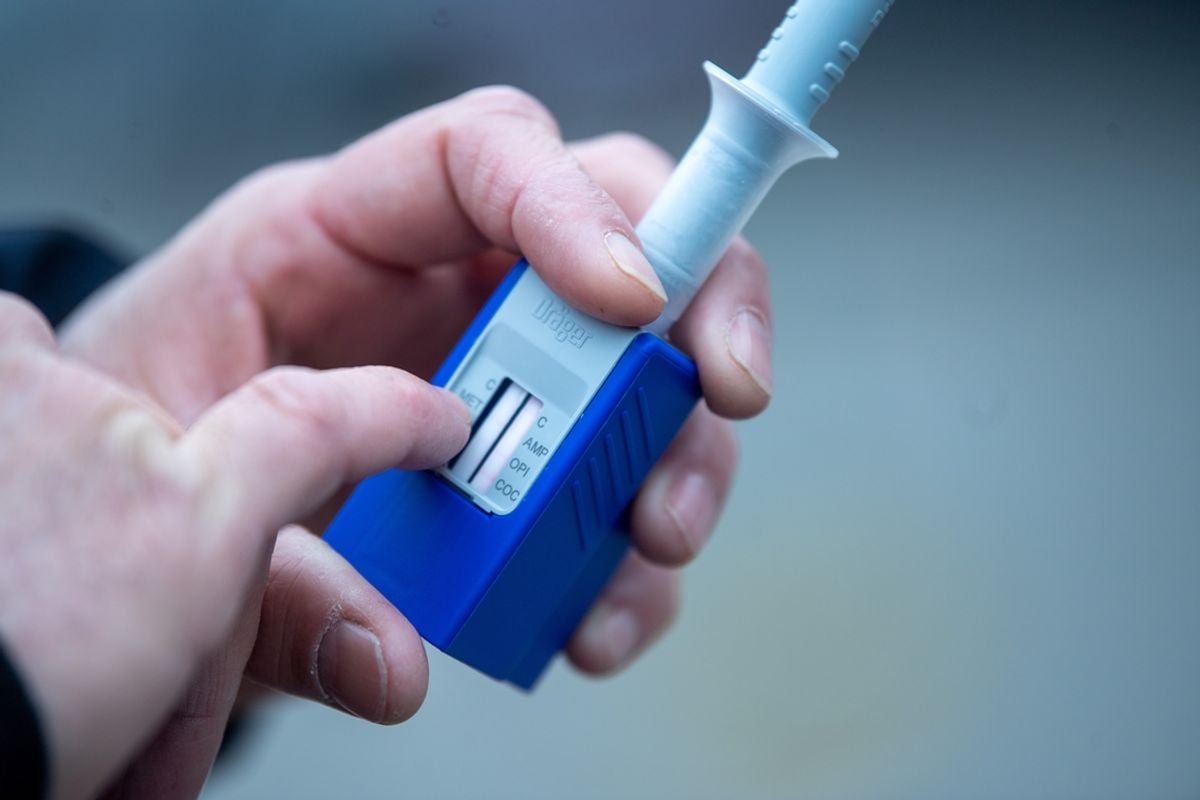
A routine roadside check turned into a nightmare for a 43-year-old patient in central France, whose prescribed painkillers triggered a positive drug test. The driver, known as Lino, relies on therapeutic morphine to manage severe illness-related pain. When officers conducted a saliva screen, the result flagged “opioids,” and his driving license was promptly seized. He insists he has never used illicit drugs and calls what followed a profound injustice.
The case exposes a fraught intersection between medical care and road safety, where tools built to catch recreational use can also ensnare patients. It raises urgent questions about how authorities weigh risk, how tests are validated, and how to protect both public safety and patients’ rights.
A routine stop with a costly aftermath
On a December morning near Clermont-Ferrand, police were conducting checks close to a known trafficking spot. Lino parked near his doctor’s office, arriving to renew a prescription for legally dispensed morphine. A quick saliva test returned positive, and officers, following standard procedure, withdrew his license. He says the officer declined to review his medical papers or appointment proof, arguing that none of it changes a positive roadside result.
Weeks later, still under treatment and needing medical care, Lino was stopped again outside the same clinic. The second test was also positive, and his license was once more removed. For a patient juggling hospital visits and shared child custody, the practical impact has been immense.
“I feel punished for being sick,” he said, voice tight with frustration. “I do everything by the book, and still I’m treated like a criminal.”
The blind spot in roadside testing
Saliva tests are designed to be fast and simple, but they often cannot distinguish between therapeutic morphine and street opioids like heroin. Experts note that a positive oral-fluid screen is a preliminary indicator, not a definitive diagnosis. A blood test can confirm the presence of morphine, yet it still cannot prove whether the source was a prescription or illicit use.
This technical limitation leaves patients vulnerable to administrative sanctions even when they follow a doctor’s orders. The device does what it’s built to do—spot a molecule—but it doesn’t assess impairment. Nor does it contextualize why that molecule is in someone’s system.
Law and medicine at cross-purposes
French road rules treat certain substances as “stupéfiants,” and their presence behind the wheel is forbidden, regardless of whether the product was legally prescribed. That legal framing focuses on substance classification, not individual impairment. It also doesn’t account for the medically supervised use of analgesics, antitussives like codeine, or related compounds that can also trigger positives.
For patients, the message is confusing: take your doctor-approved medicine, but don’t drive if it can light up a test—even if you feel fit to drive. For authorities, the imperative is clear: reduce risk on the roads, even if the tools are blunt and the fallout for patients can be harsh.
“It’s an injustice”: the human toll
Lino says he now must rely on others for essential appointments, including oncology care far from home. The loss of autonomy is not just inconvenient; it threatens continuity of treatment and family stability. “It is simply not right to criminalize people who are ill,” he said. “I want the system to see the difference between therapy and abuse.”
Legal specialists in road law acknowledge recurring cases like Lino’s and say drivers are often unaware that they can request confirmatory blood tests. Even then, experts caution that blood results may not exonerate a patient when the law is written to penalize the substance’s mere presence.
What would make the system fairer?
- Clear, uniform roadside guidance that informs drivers on prescriptions of their right to request a confirmatory blood test.
- Laboratory protocols that document therapeutic use (e.g., prescription verification) alongside toxicology results.
- Statutory reform distinguishing legal therapeutic possession from illicit drug consumption, with impairment-based criteria.
- Health-passport style documentation linking active prescriptions to test results, reducing wrongful administrative sanctions.
Practical realities for patients on opioids
Until laws and tools evolve, patients face a patchwork of practical choices. Clinicians can flag driving risks and, where possible, adjust dose timing to minimize overlap with driving hours. Patients can carry recent prescriptions and appointment proofs, though those may not alter an on-the-spot decision. And if stopped, they can calmly request confirmatory testing, documenting every step for later review.
The broader tension is not going away: road safety is a genuine priority, but so is protecting people who take medicine as directed. Without a better scientific and legal bridge, more patients will fall into this gap. Lino’s case underlines a simple truth: a system that cannot tell treatment from transgression will keep producing preventable harm—and eroding trust among those who most need care.